Issue 3 · Volume 55 · March 2023
Hormone and Metabolic Research 2023年第3期现已上线,欢迎免费阅读本期三篇精选论文。
Original Article: Endocrine Care
Papillary Thyroid Microcarcinoma: Insights from a Cohort of 257 Thyroidectomized Patients
Henrique Cabral Scherer, Paula Martins Fernandes, Rafael Selbach Scheffel, André Borsatto Zanella, Ana Luiza Maia, Jose Miguel Dora
Papillary thyroid microcarcinoma management evolved, and less aggressive strategies are now considered. Questions, however, remain on these tumors’ behavior, particularly on developing countries' real ground healthcare scenarios. Our aim is to gather insights on the natural history of papillary thyroid microcarcinoma on patients treated with thyroidectomy in Brazil. Consecutive patients diagnosed with papillary thyroid microcarcinoma had their clinical characteristics, interventions, and outcomes described. Patients were classified as incidental or nonincidental based on the diagnosis after or before surgery, respectively. A sum of 257 patients were included, 84.0% of which were women, and the mean age was of 48.3±13.5 years. The mean tumor size was of 0.68±0.26 cm, 30.4% were multifocal, 24.5% had cervical metastasis, and 0.4% distant metastasis. The nonincidental and incidental tumors differed in tumor size (0.72±0.24 and 0.60±0.28 cm, respectively, p=0.003) and in presence of cervical metastasis (31.3% and 11.9%, respectively, p<0.001). Male sex, nonincidental diagnosis, and younger age were independent predictors of cervical metastasis. After 5.5 years (P25–75 2.5–9.7) of follow-up, only 3.8% of patients had persistent structural disease (3.4% cervical). Predictors of persistent disease at multivariate analysis included cervical metastasis and multicentricity. In conclusion, incidental and nonincidental papillary thyroid microcarcinoma patients of the population studied displayed excellent outcomes. Cervical metastasis and multicentricity were frequent findings and prognostic factors for persistent disease.
Original Article: Endocrine Care
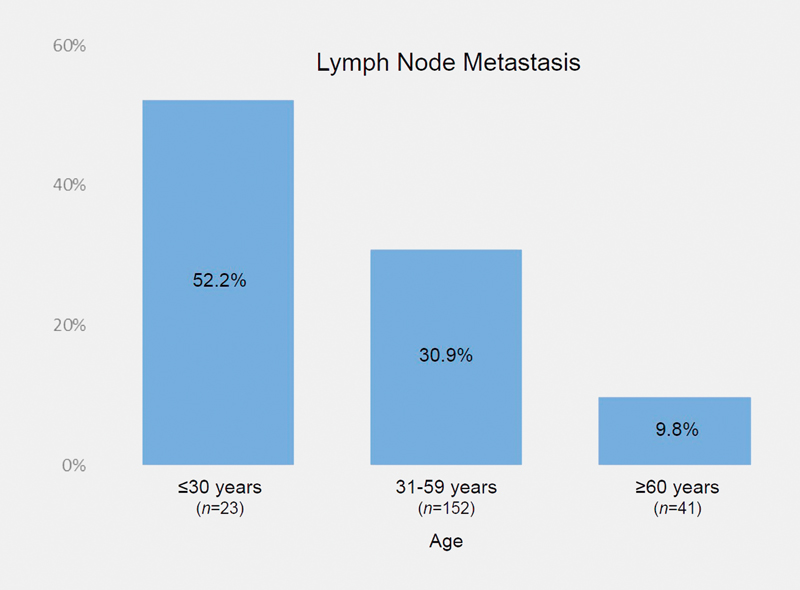
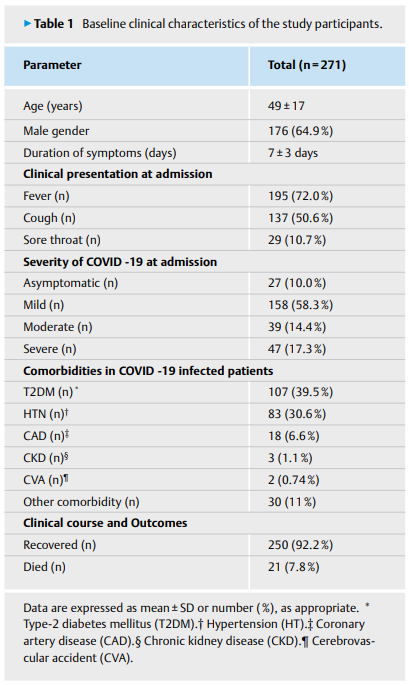
Deepika Patel, Dukhabandhu Naik, Sadishkumar Kamalanathan, Kadhiravan Tamilarasu, Jayaprakash Sahoo, Ayan Roy, Chandhana Merugu, Varun Suryadevara
Thyroid gland can be affected by the COVID-19 infection. The pattern of thyroid function abnormality reported in COVID-19 is variable; in addition, some drugs used in COVID-19 patients like glucocorticoids and heparin can affect the thyroid function tests (TFT). We conducted an observational, cross-sectional study of thyroid function abnormalities with thyroid autoimmune profile in COVID-19 patients with varying severity from November 2020 to June 2021. Serum FT4, FT3, TSH, anti-TPO, and anti-Tg antibodies were measured before the initiation of treatment with steroids and anti-coagulants. A total of 271 COVID-19 patients were included in the study, of which 27 were asymptomatic and remaining 158, 39, and 47 were classified to mild, moderate and severe categories, respectively, according to MoHFW, India criteria. Their mean age was 49±17 years and 64.9% were males. Abnormal TFT was present in 37.2% (101/271) patients. Low FT3, low FT4, and low TSH were present in 21.03%, 15.9% and 4.5% of patients, respectively. Pattern corresponding to sick euthyroid syndrome was the most common. Both mean FT3 and FT3/FT4 ratio decreased with increasing severity of COVID-19 illness (p=0.001). In multivariate analysis, low FT3 was associated with increased risk of mortality (OR 12.36, 95% CI: 1.23–124.19; p=0.033). Thyroid autoantibodies were positive in 58 (27.14%) patients; but it was not associated with any thyroid dysfunction. Thyroid function abnormality is common among COVID-19 patients. Both low FT3 and FT3/FT4 ratio are indicators of disease severity while low FT3 is a prognostic marker of COVID-19 associated mortality.
Original Article: Endocrine Care
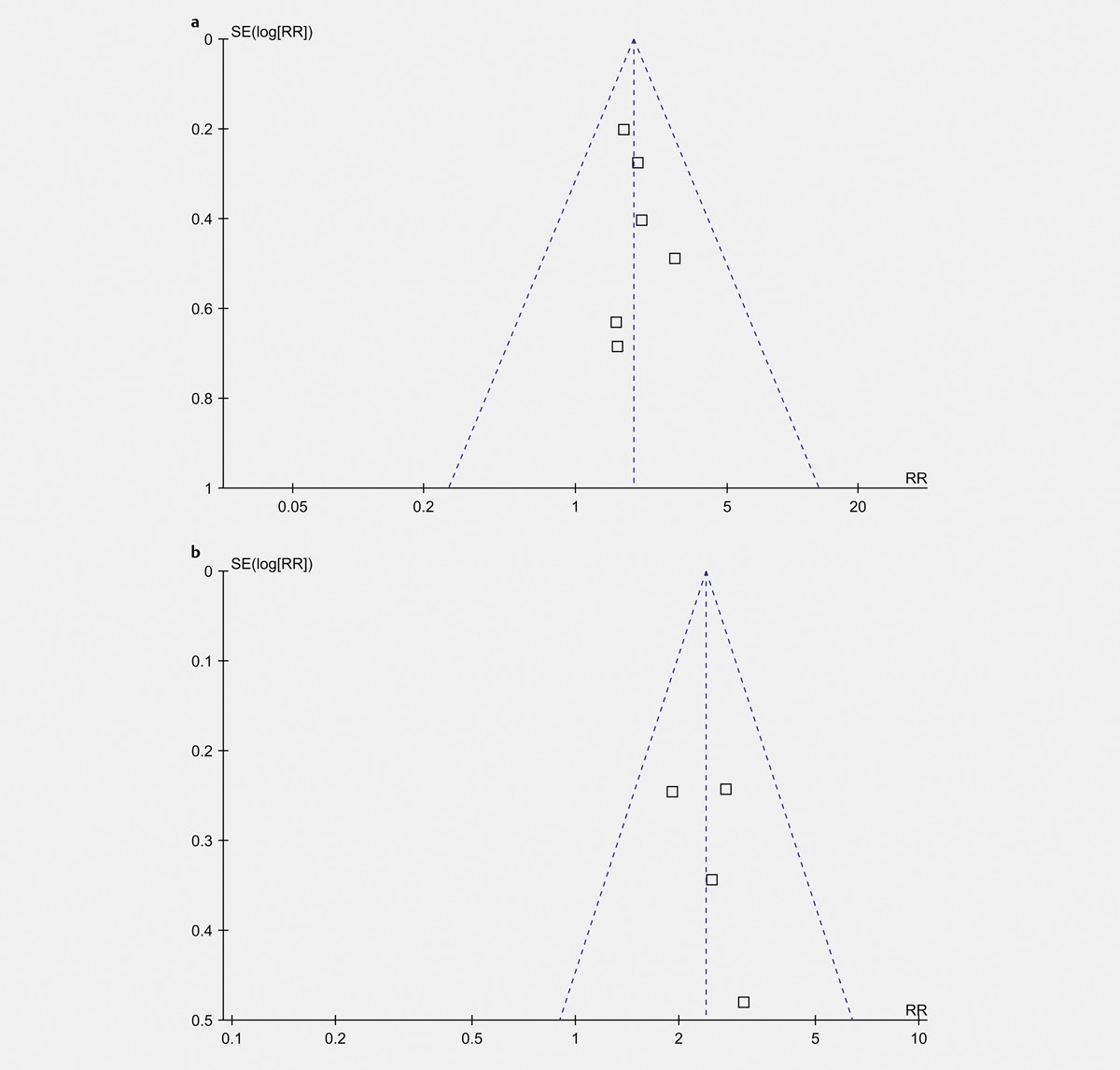
Glycemic Variability and Prognosis of Patients with Intracerebral Hemorrhage: A Meta-Analysis
Xu Jiao, Huifang Wang, Mingfei Li, Yun Lu
Glycemic disorder may affect the outcomes of patients with intracerebral hemorrhage (ICH). However, the association between glycemic variability (GV) and prognosis in these patients remains to be determined. We performed a meta-analysis to compressive the influence of GV on functional outcome and mortality in patients with ICH. Observational studies comparing the risks of poor functional outcome (defined as modified Rankin Scale>2) and all-cause mortality between ICH patients with higher versus lower acute GV were retrieved by systematic search of Medline, Web of Science, Embase, CNKI, and Wanfang databases. A random-effect model was used to pool the data after incorporating the between-study heterogeneity. Sensitivity analyses were performed to evaluate the stability of the findings. Eight cohort studies involving 3400 patients with ICH were included in the meta-analysis. The follow-up duration was within 3 months after admission. All of the included studies used standard deviation of blood glucose (SDBG) as the indicator of acute GV. Pooled results showed that ICH patients with higher SDBG were associated with a higher risk of poor functional outcome as compared to those with lower SDBG [risk ratio (RR): 1.84, 95% confidence interval (CI): 1.41 to 2.42, p<0.001, I2=0%]. In addition, patients with higher category of SDBG were also associated with a higher mortality risk (RR: 2.39, 95% CI: 1.79 to 3.19, p<0.001, I2=0%). In conclusion, high acute GV may be a predictor of poor functional outcome and mortality of patients with ICH.