

Thieme小儿科学期刊European Journal of Pediatric Surgery的影响因子2020提高到了2.191。非常感谢所有作者、审稿人和编辑的支持和最宝贵的贡献。
以下三篇是被引用次数最多的论文,它们对影响因子的提高有着重要贡献,欢迎免费阅读。
State of Play: Eight Decades of Surgery for Esophageal Atresia
Zimmer et al.
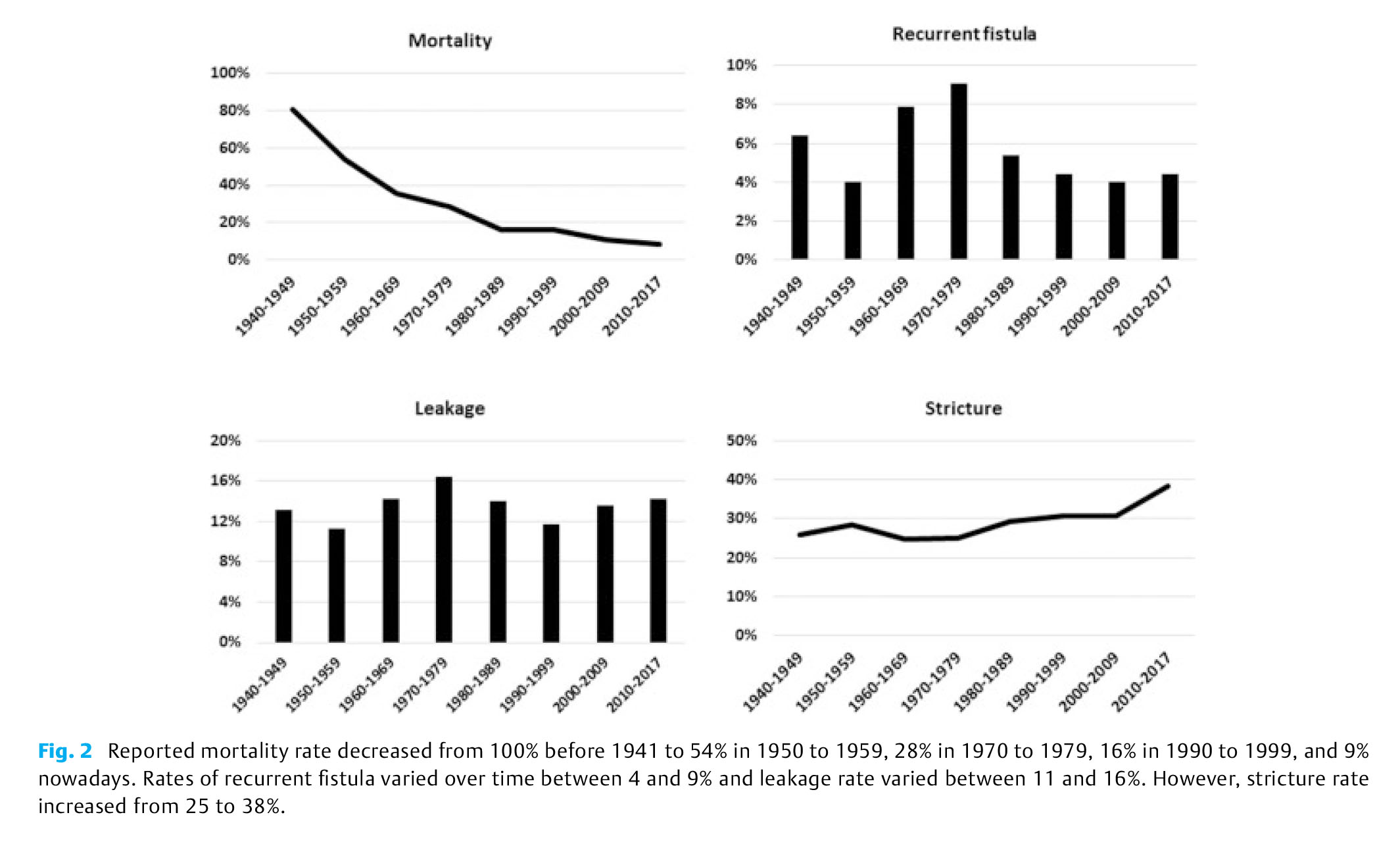
Aim: Surgical expertise and advances in technical equipment and perioperative management have led to enormous progress in survival and morbidity of patients with esophageal atresia (EA) in the last decades. We aimed to analyze the available literature on surgical outcome of EA for the past 80 years.
Materials and Methods: A PubMed literature search was conducted for the years 1944 to 2017 using the keywords “esophageal/oesophageal atresia,” “outcome,” “experience,” “management,” and “follow-up/follow up.” Reports on long-gap EA only, non-English articles, case reports, and reviews without original patient data were excluded. We focused on mortality and rates of recurrent fistula, leakage, and stricture.
Results: Literature search identified 747 articles, 118 manuscripts met the inclusion criteria. The first open end-to-end anastomosis and fistula ligation was reported in 1941. Thoracoscopic fistula ligation and primary anastomosis was performed first in 2000. Reported mortality rate decreased from 100% before 1941 to 54% in 1950 to 1959, 28% in 1970 to 1979, 16% in 1990 to 1999, and 9% nowadays. Rates of recurrent fistula varied over time between 4 and 9%. Leakage rate remained stable between 11 and 16%. However, stricture rate increased from 25 to 38%.
Conclusion: Including a full range of articles reflecting the heterogeneity of EA, mortality rate significantly decreased during the course of 80 years. Along with the decrease in mortality, there is a shift to the importance of major postoperative complications and long-term morbidity regardless of surgical technique.
The Global Initiative for Children's Surgery: Optimal Resources for Improving Care
Goodman et al.
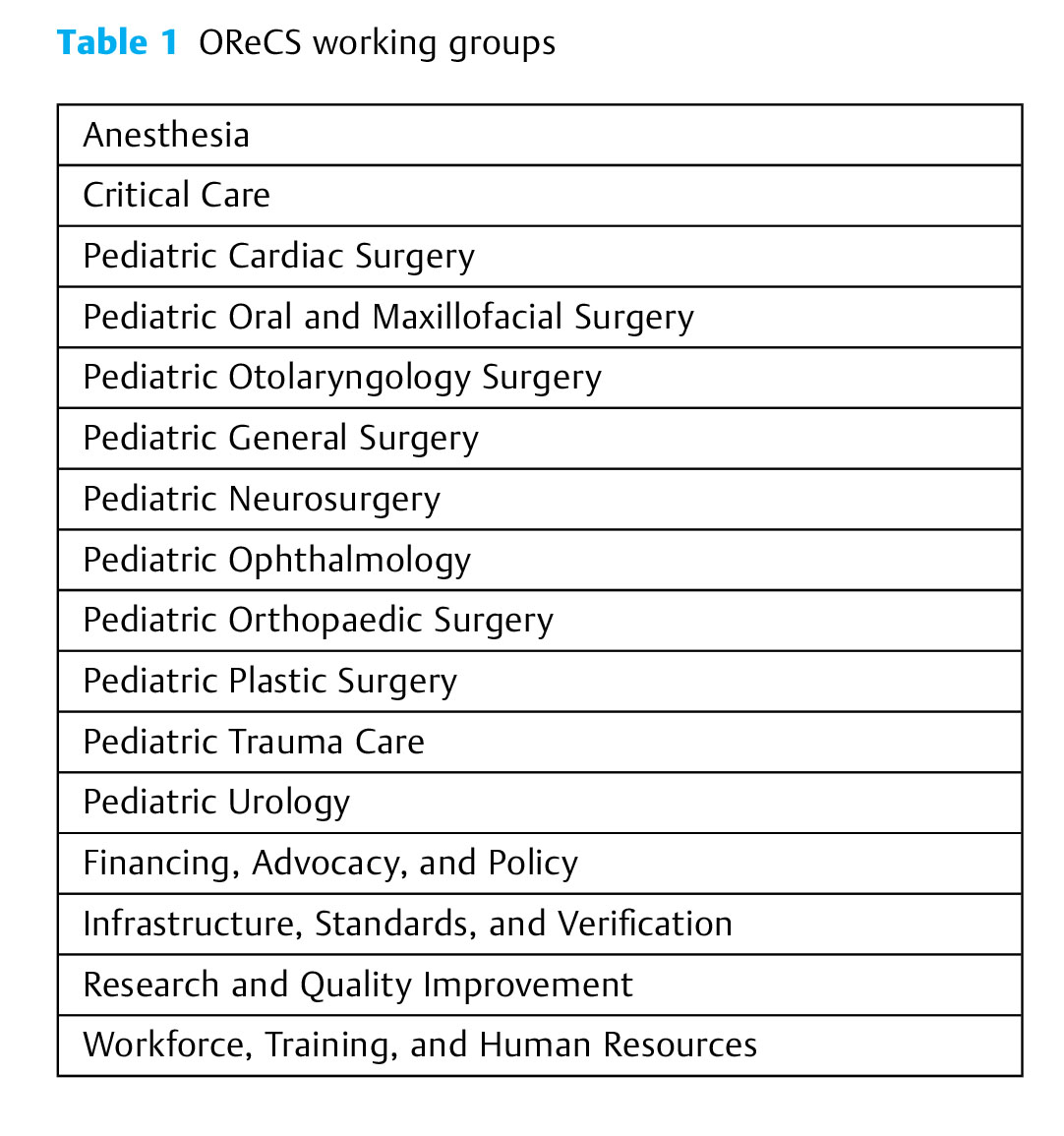
Background: The Lancet Commission on Global Surgery reported that 5 billion people lack access to safe, affordable surgical care. The majority of these people live in low-resource settings, where up to 50% of the population is children. The Disease Control Priorities (Debas HTP, Donkor A, Gawande DT, Jamison ME, Kruk, and Mock CN, editors. Essential Surgery. Disease Control Priorities. Third Edition, vol 1. Essential Surgery. Washington, DC: World Bank; 2015) on surgery included guidelines for the improvement of access to surgical care; however, these lack detail for children's surgery.
Aim: To produce guidance for low- and middle-income countries (LMICs) on the resources required for children's surgery at each level of hospital care.
Methods: The Global Initiative for Children's Surgery (GICS) held an inaugural meeting at the Royal College of Surgeons in London in May 2016, with 52 surgical providers from 21 countries, including 27 providers from 18 LMICs. Delegates engaged in working groups over 2 days to prioritize needs and solutions for optimizing children's surgical care; these were categorized into infrastructure, service delivery, training, and research. At a second GICS meeting in Washington in October 2016, 94 surgical care providers, half from LMICs, defined the optimal resources required at primary, secondary, tertiary, and national referral level through a series of working group engagements.
Results: Consensus solutions for optimizing children's surgical care included the following:
Establishing standards and integrating them into national surgical plans.
Each country should have at least one children's hospital.
Designate, facilitate, and support regional training hubs covering all children's surgical specialties.
Establish regional research support centers.
An “Optimal Resources” document was produced detailing the facilities and resources required at each level of care.
Conclusion: The Optimal Resources document has been produced by surgical providers from LMICs who have the greatest insight into the needs and priorities in their population. The document will be refined further through online GICS Working Groups and the World Health Organization for broad application to ensure all children have timely access to safe surgical care.
Morini et al.
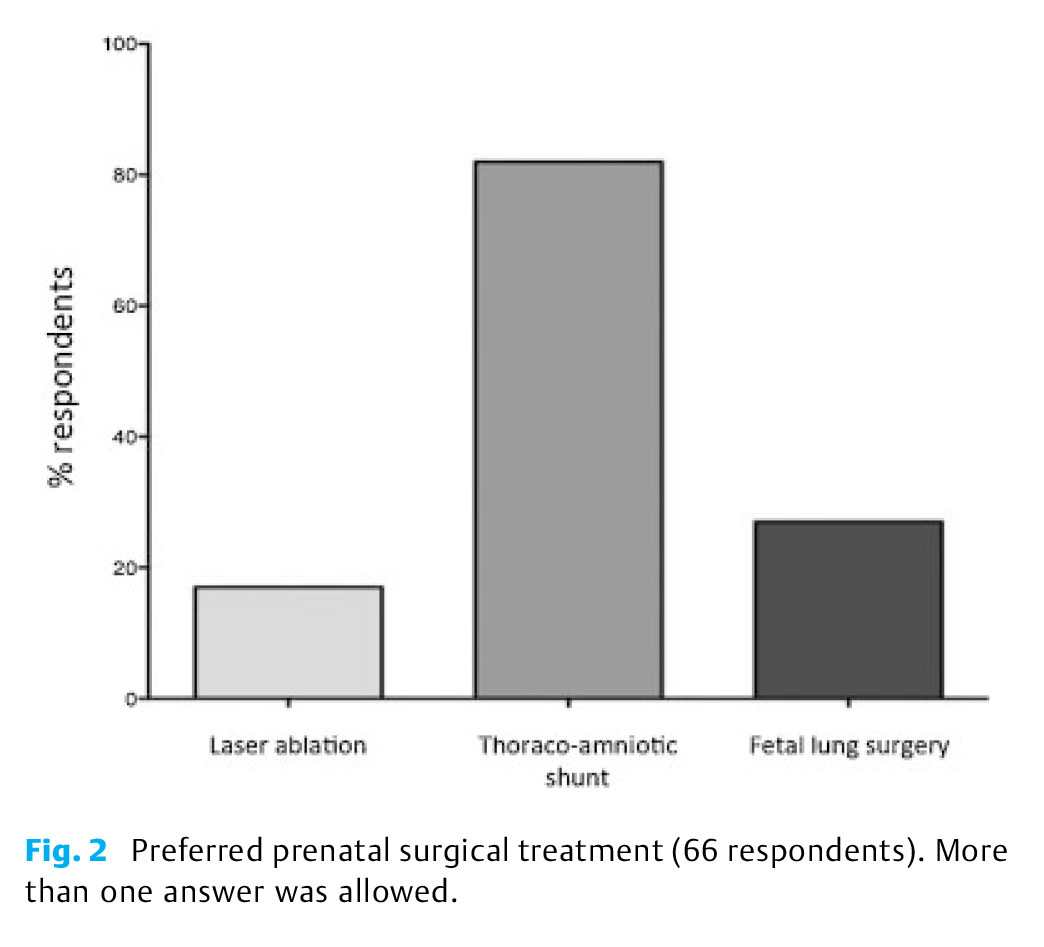
Aim: To define current management of congenital pulmonary airway malformation (CPAM).
Methods: A total of 181 European Pediatric Surgeons' Association members (91% senior) from 48 countries completed an online questionnaire.
Main Results: Prenatal: 93% respondents work in centers with prenatal diagnosis facilities, and 27% in centers offering in utero surgery. Prenatal counseling is performed by 86% respondents, 22% of whom see >10 cases per year. Risk of single pre-/postnatal complications is deemed low (<5%) by more than 60% of respondents. Eighty-six percent respondents do not offer pregnancy termination for prenatally diagnosed CPAM. Fetal hydrops is the most frequent indication for termination (87%), followed by parental willingness (52%). Prenatal surgery is an option for 44% respondents, preferring thoracoamniotic shunt (82%).
Postnatal: 75% respondents operate on asymptomatic patients, 18% before 6 months of age, 62% between 6 and 12 months of age, and 20% after 12 months of age. Risk of infection (86%), cancer (63%), and symptoms development (62%) are indications for surgery in asymptomatic CPAM. Sixty-three percent prefer a thoracotomy. Lobectomy is the preferred procedure (58% respondents). Motivations against surgery include lesion <1 cm (64%), risk of postoperative complications (37%), and lack of evidence favoring surgery (27%). Seventeen percent respondents have seen at least one patient with CPAM with lung cancer, in 89% of the cases within the CPAM. Of all the respondents, 83% and 22% offered dedicated follow-up and genetic screening, respectively.
Conclusion: Current pre- and postnatal management of CPAM lacks uniformity, particularly for surgical indication, timing, and approach. Efforts should be made toward standardization. Risk of CPAM-associated cancer is not clear.
阅读本刊更多论文,请点击这里。
